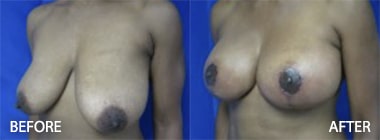
Complications of Breast Augmentation
Complications of breast augmention surgery include hematoma, seroma, wound infection, and permanent alterations in nipple sensation. (In Dr. Hughes’s extensive experience, these represent less than 1% of cases).
Implant complications include displacement, rippling, and rupture.
Hematoma development after breast augmentation has both short-term effects (pain, disfigurement, blood loss) and long-term consequences (capsular contracture). The best treatment of hematoma development is prevention. Should a hematoma develop, prompt evacuation and copious irrigation should be utilized.
Wound infections can range from mild cellulitis of the breast skin to a purulent periprosthetic space infection. The most frequently identified pathogen is Staphylococcus epidermidis. Infections should be treated early, when they are typically responsive to antibiotics rather than to let the infection go unchecked to the point where the implant has to be removed. However, removal of implants has been reported in aggressive infections. Although this complication has not been observed by Dr. Hughes, this may occur in 1% of cases.
Persistent seromas may require aspiration or, for refractory cases, placement of drainage catheters.
The periareolar approach is generally associated with the highest rate of changes in nipple sensation. However, this has less to do with the incision and more to do with the dissection.
The most common implant-related complication remains implant displacement with subsequent breast asymmetry. This complication ranks second only to capsular contracture as the major source of dissatisfaction. Rippling may be observed in both saline and silicone implants. This may be more prominent in saline implants, but rippling usually occurs after a period of years after breast augmentation as the breast tissue is thinned by the implant. Silicone is regarded to have less rippling. However, changing the implant is frequently not enough, and the revision breast augmentation may require fat grafting or placement of a dermal matrix to camouflage the implant. To read more about dermal matrices go to the Dermal Matrices in Breast Augmentation (2012) chapter written by Dr. Hughes.
Article 2: The Evolution of Saline and Textured Implants
Article 3: Silicone Implants and Implant Controversies
Article 4: Evaluation of the Breast Augmentation Surgery Patient
Article 5: Determining Implant Size and Incisions in Breast Augmentation: Inframammary and Infraareolar
Article 6: Incisions and Approaches to Breast Augmentation: Transaxillary and Transumbilical
Article 7: Capsular Contracture in Breast Augmentation
Article 8: Complications of Breast Augmentation