AAAASF or QuadA Sets the Gold Standard for Surgical Center Accreditation
The American Association for Accreditation of Ambulatory Surgery Facilities, Inc. (AAAASF) was established 40 years ago to standardize and improve the surgical care in outpatient facilities. Surgeons, health agencies, and patients acknowledge that AAAASF sets the gold standard
Dr. Kenneth Hughes and his team of architects, engineers, and physicists set out to create a true state of the art surgery center with meticulous attention to details, patient safety, and infection control. The operating room contains a custom air handler that cycles the entire circulating volume of the operating room 20 times an hour, which means a continuous flow of clean, purified air. The operating room is equipped with ultraviolet light beams that kill microorganisms. Finally, the air is filtered by a MERV 13 filter that removes bacteria and smaller particles from the air. This tripartite system assures that the patient will have the smallest possible probability of acquiring an infection.
All of the operating room equipment and recovery room equipment has been individually selected for quality and reliability and has been meticulously inspected and certified. Emergency backup power provides for full function and safety for the patient, no matter what the surgery or its duration, even in the exceptionally rare case of power outage. This system will keep everything fully functional for 8 hours, which is greater than medicare standards.
All gases to the operating room are piped and routed from fire rated storage shelters, so that the operating room will be safe from anesthetic gases and other flammable substances. The surgery center is fully ADA compliant and our facility is fully compliant with CA title 24 energy conservation legislation. We have the latest sensor systems and advanced LED technology to control lighting to fit the needs of the patients and surgical staff in an energy efficient manner. The entire structure is surrounded by steel girders that will withstand 8.0 earthquakes and other natural disasters.
Dr. Kenneth Hughes not only has the best and newest equipment in his operating room and recovery areas, but he has backups for virtually everything. He has a brand new anesthesia machine for the rarest situation that an anesthesia machine becomes defunct, nonfunctional, or dead during any operation. This other anesthesia machine can simply be connected in less than a minute. Dr. Kenneth Hughes also has an additional, fully functional operating table within the office that can be used if there is any problem with the current operating table. If the power to the city is lost or turned off, the surgery center has the ability to operate for an 8 additional hours without disruption. The surgery center has multiple new defibrillators, which are checked daily for functionality. Dr. Kenneth Hughes has crash cart medications that are up to date and checked daily. The center also has duplicate medications for the rare instance that all of the medications are used on one day.
Dr. Hughes uses board-certified, hospital staff anesthesiologists to provide the highest level of care possible along with potential overlap in personnel if necessary. These individuals are all experienced and highly skilled and are capable of managing any high stress situation. They have experience in emergency and critical care situations and preserve their skills by retaining their hospital positions, performing codes for patients at risk of death from heart attack, stroke, or embolus who require ACLS (advance cardiac life support) and beyond.
Dr. Kenneth Hughes has spared no expense to create the safest environment for his patients. The surgery center has been fully accredited with AAAASF (The American Association for Accreditation of Ambulatory Surgery Facilities, Inc.) until 2026 and meets or exceeds all standards.
Types of Surgeries Performed in Dr. Kenneth Hughes’s Fully Accredited Surgery Center in Los Angeles
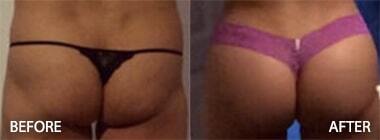
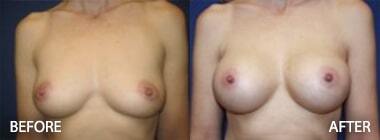
Dr. Hughes performs a broad array of plastic, reconstructive and cosmetic surgery procedures. He performs some virtually scarless or low scar burden procedures including short scar face lift, facial fat grafting, closed rhinoplasty (no visible external scars), chin implants with no external scar, short scar tummy tuck, and TUBA (breast augmentation without scars on your breasts).
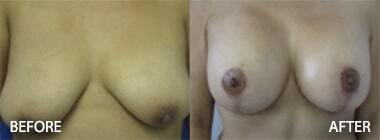
In addition, he performs breast augmentations through any incision possible as well as natural breast augmentation with breast fat grafting and breast fat transfer techniques. Dr. Hughes performs additional breast surgeries such as breast lifts, breast reductions, and breast asymmetry corrections as well as breast reconstructions.
Dr. Hughes performs the full spectrum of facial surgeries including rhinoplasties, facial fat grafting, brow lifts, face lifts, upper and lower eyelid surgeries, and chin implants. He has also performed thousands of body plastic surgery procedures including liposuction/liposculpture, tummy tucks, Brazilian butt lifts or BBLs and butt implant surgeries, mommy makeovers, arm lifts, thigh lifts, labial rejuvenation, vaginoplasty, fat necrosis removal, and silicone injection removal.
Finally, Dr. Kenneth Hughes has become a world renowned expert in revision and combination surgery. Dr. Hughes routinely performs liposuction revision with and without Bodytite, Brazilian buttlift revision, as well as hundreds of facelift and rhinoplasty revisions along with breast implant and breast lift revisions.
- DIAGNOSTIC TESTING: Know your COVID-19 diagnostic testing availability, and develop operational testing policies for patients and health care workers.
- Know, understand, and update your local COVID-19 diagnostic testing capabilities and turnaround times. The testing availability will likely change during the ramp-up period. While it is to be hoped that availability is on the rise, some predict that availability may actually decrease as the community testing demands increase.
- Develop local diagnostic testing policies for patients. Rapid testing for COVID-19 infection through real-time reverse transcription polymerase chain reaction (RT-PCR) testing may be considered for all patients undergoing planned surgery, or for selected patients after screening with or without mandatory preoperative quarantine. The prevalence of asymptomatic/presymptomatic patients is unknown, but likely varies according to the pretest probability, i.e., prevalence of disease in the community. Surgeons should be involved in institutional policymaking since the risk to the patient and the staff varies with the type of procedure, the patient’s condition, local circumstances, and over time. Some surgeon discretion is necessary and should be permitted.
- Develop diagnostic screening testing policies for health care workers. With near-future reversal of physical distancing, local incidence may increase, including among health care workers. As ramp up proceeds, screening and testing policies and planning for staff should be considered.
II. Preparedness
- PERSONAL PROTECTIVE EQUIPMENT:
- PPE supplies: Stored inventory—or a reliable supply chain—of PPE for both airborne/aerosol and droplet/contact precautions optimally for at least 30 days of operations should exist in a hospital prior to relaxing restrictions on surgical activity.
- LOCAL FACILITY CAPACITY: Know your health care facility capacity (e.g., beds, ICUs, ventilators), including capacity in expansion strategies (e.g., weekends).
- The approach to restoring the elective surgery caseload depends greatly on the hospital’s available resources, including OR capacity and alternative sites of care. Sufficient facility capacity for providing care to surgical patients must be present in the system, including—in addition to ORs and peri-anesthesia units—critical care, emergency, diagnostic imaging, and laboratory services.
- Consider potential sites for resuming elective surgery, including those facility areas that were converted or closed during the surge, such as ORs, ambulatory surgery centers, and hospital outpatient departments.
- Facility cleaning policies in context of COVID-19 should be considered. Cleaning—in all areas—along the continuum of care should be addressed (e.g., clinic, preoperative, ORs, workrooms, recovery room, ventilators, etc.).
- Certain select procedures may be appropriate for the office setting as long as safety concerns are identified and addressed.
- The OR schedules should change to accommodate the rapid influx of cases. Modifications may include limiting block time assignments to increase open time and extending hours of elective operations later into the evening and on the weekends.
- Ensure that a post-corona elective surgery surge will not overwhelm the local facility throughout preoperative, intraoperative, postoperative, and post-acute care phases.
- RESOURCES AND SUPPLIES: Supply chain/support areas.
- A resumption to normal levels of surgical supplies, implants, and equipment must be in place prior to reactivating elective surgery and commensurate with anticipated ramp-up procedures (e.g., anesthesia-sedation medications, PPEs, other).
- Ensuring a supply of products is available from traditional or new vendors as well as vendor support is necessary.
- ORs should take inventory of existing supplies for the particular service lines, prioritized with a focus on those with expiration dates.
- Cleaning supplies for all areas where COVID-19 or PUI patient care was/is being delivered.
- HEALTH CARE WORKERS: Workforce staffing issues.
- Multidisciplinary staffing coverage for routine and “expanded” hours.
- Ensure coordination among surgery, anesthesia, nursing, engineering, housekeeping, and others.
- Consider creating and/or updating PPE policies to protect workers from a new infection.
- Contingency planning in potential situation of newly diagnosed health care workers.
- Ensure adequate health care worker staffing to accommodate a COVID-19 surge if a second wave occurs.
- REVIEW-GOVERNANCE COMMITTEE: Assign a governance committee to clarify, interpret, and iterate policies, make real-time decisions, and initiate and communicate messaging.
- Function: Real-time governance, decision-making body
- Members: Multidisciplinary (e.g., surgery, anesthesia, nursing, others)
- Frequency: At least daily huddles during ramp-up period and possibly beyond
- Data-driven, e.g., utilization, efficiency, COVID-19 awareness data, errors/near misses, complications.
III. Patient Issues
- PATIENT COMMUNICATION: Surgery patients may have myriad questions and concerns regarding the ramp-up period. Clear messaging and communication will be paramount.
- Potential messaging-communication topics include:
- Procedure prioritization
- COVID-19 testing policies for patients
- COVID-19 counseling
- Safety for patients receiving care within the health care system—facilities, health care workers
- PPE use
- Patient family/visitor guidelines
- Postdischarge care/follow-up
- Transparency of the principles, framework, and prioritization process to hospitals, surgeons, patients, and the public will provide assurance, consistency, and reliability, as it will help to standardize the integration of decision-making factors not usually considered in clinical judgment outside the pandemic/postpandemic setting. It also will help to reduce ethical dilemmas and potential for moral injury for surgeons, anesthesiologists, nursing, surgical leadership, and others.
- During development of the local prioritization process, the following may be considered:
- Consider local strategies for increasing “OR time” availability, e.g., weekends, extended hours (see following for issues related to OR expansion).
- Supply chain.
- PPE availability.
- Establish review-governance committee, see above, to review such issues as process of prioritization for ORs.
- The prioritization process and criteria may vary in real time according to institutional resources, capabilities, business priorities, and other issues. Issues in question should be evaluated in concert with the governance committee.
- Issues to consider associated with increased OR volume/OR expansion:
- Ensure primary personnel availability commensurate with increased OR volume/OR hours (e.g., surgeon, anesthesia, nursing, housekeeping, engineering, etc.)
- Ensure supply availability (e.g., medications, suture)
- Ensure ventilator availability
- New staff training
- Potential messaging-communication topics include:
IV. Delivery of Safe and High-Quality Care
- Ensuring safe, high-quality, high-value care of the surgical patient across the Five Phases of Care continuum.
- Utilize quality improvement programs/care standards to help support achieving safe, high-quality, high-value patient care.
- Use of risk-adjusted data to evaluate patient care and outcomes.
- Ensure optimal patient care across Five Phases of Care:
- Phase I: Preoperative period
- Consider guideline for repeating laboratory results, radiology, history and physical, re-consent vs. use of prior results.
- Consider use of telehealth.
- Consider guideline to (re)assess comorbidities especially if COVID-19/PUI or extended length of time of postponed operation.
- Consider use of telehealth.
- The composite assessment, in conjunction with sound clinical judgment, provides the surgeon and other decision makers with the information needed to make decisions regarding clinical appropriateness as well as surgical prioritization.
- Office, clinic, hospital public areas (e.g., waiting room) should continue to practice physical distancing (e.g., six-feet spacing of chairs)
- Consider review of patient advance directive, especially older adults, frail, COVID-19+, other.
- Evaluate and discuss patient’s potential need for post-acute care facility (rehabilitation medicine, skilled nursing facility, other) before operation (given known COVID-19 outbreaks in post-acute care-type facilities).
- Preoperative setting (e.g., clinic, office, or non-COVID-19 care (NCC) areas) should consider screening all patients before the appointment for symptoms of COVID-19 disease, including temperature checks, and routinely screen all staff and others who would be working in the facility (physicians, nurses, housekeeping, delivery, and others).
- As stated above in PPE section, aligning with CDC and CMS recommendations, consider a policy for all health care providers and staff to wear surgical face masks at all times. Procedures on the mucous membranes, including the respiratory tract, that have a higher risk of aerosol transmission should be done with great caution, and staff should utilize appropriate respiratory protection such as N95 masks and face shields.
- Patients should wear a cloth face covering that can be bought or made at home.
- Consider guideline for repeating laboratory results, radiology, history and physical, re-consent vs. use of prior results.
- Phase II: Immediate Preoperative Period
- Review nursing, anesthesia, surgery checklists for potential need to be revised re: COVID-19+, other?
- Phase III: Intraoperative Period
- Review whether time-outs and briefings need revision with regard to COVID-19 risk, COVID-19 testing results, and ensure PPE use guidelines are being followed.
- Consider guideline for personnel to be present during intubation, and consider including waiting time (e.g., with regard to air circulation cycling time) before beginning operation.
- PPE use guideline (see above).
- Review specimen pick-up protocol.
- Phase IV: Postoperative Period
- Adhere to standardized care protocols as much as possible (e.g., enhanced recovery protocols) for increased reliability in light of potential different personnel as standardized protocols optimize lengths of hospital stay and efficiency and are associated with decreased complication rates.
- Phase V: Post Discharge Period
- Post-acute care facility availability.
- Post-acute care facility safety (COVID-19, non-COVID-19 issues).
-
3. Personal Protective Equipment
4. Case Prioritization and Scheduling
Principle: Facilities should establish a prioritization policy committee consisting of surgery, anesthesia and nursing leadership to develop a prioritization strategy appropriate to the immediate patient needs.
Considerations: Prioritization policy committee strategy decisions should address case scheduling and prioritization and should account for the following:
- Strategy for allotting daytime “OR/procedural time” (e.g., block time, prioritization of case type [i.e., potential cancer, living related organ transplants, etc.]).
- Identification of essential health care professionals and medical device representatives per procedure.
- Strategy for phased opening of operating rooms.
- Identify capacity goal prior to resuming 25% vs. 50%
- Outpatient/ambulatory cases start surgery first followed by inpatient surgeries.
- All operating rooms simultaneously – will require more personnel and material.
- Strategy for increasing “OR/procedural time” availability (e.g., extended hours before weekends).
- Issues associated with increased OR/procedural volume.
5. Post-COVID-19 Issues for the Five Phases of Surgical Care
Principle: Facilities should adopt policies addressing care issues specific to COVID-19 and the postponement of surgical scheduling.
Considerations:
Facility policies should consider the following when adopting policies specific to COVID-19 and the postponement of surgical scheduling:
- Phase I: Preoperative
- Guideline for preoperative assessment process.
- Patient readiness for surgery can be coordinated by anesthesiology-led preoperative assessment services.
- Guideline for timing of re-assessing patient health status.
- Special attention and re-evaluation are needed if patient has had COVID‑19-related illness.
- A recent history and physical examination within 30 days per Centers for Medicare and Medicaid Services (CMS) requirement is necessary for all patients. This will verify that there has been no significant interim change in patient’s health status.
- Consider use of telemedicine for components of the preoperative patient evaluation.
- Assess preoperative patient education classes vs. remote instructions
- Guideline for preoperative assessment process.
- Phase II: Immediate Preoperative
- Guideline for pre-procedure interval evaluation since COVID-19-related postponement.
- Assess need for revision of nursing, anesthesia, surgery checklists regarding COVID‑19.
- Phase III: Intraoperative
- Assess need for revision of pre-anesthetic and pre-surgical timeout components.
- Guideline for who is present during intubation and extubation.
- Guideline for PPE use.
- Guideline for presence of nonessential personnel including students.
- Phase IV: Postoperative
- Adhere to standardized care protocols for reliability in light of potential different personnel. Standardized protocols optimize length of stay efficiency and decrease complications (e.g., ERAS).
- Phase V: Post Discharge Care Planning
- PAC facility availability.
- PAC facility safety (COVID-19, non-COVID-19 issues).
- Home setting: Ideally patients should be discharged home.Home setting.
Considerations:
- Each facility’s social distancing policy should account for:
- Then-current local and national recommendations.
- The number of persons that can accompany the procedural patient to the facility.
- Whether visitors in periprocedural areas should be further restricted.Joint Statement: Roadmap for Resuming Elective Surgery after COVID-19 Pandemic
- Phase I: Preoperative period

Dedicated operating room air handler 2

Emergency Power

merv 13 filter comparisons

Nitrous Oxide, Oxygen, Medair, and Suction Confinement

State of the Art Operating Room 300 square feet

UV light filters

Dedicated operating room air handler

Integrated UV unit within HVAC

merv 13 filters

Spacious Patient Recovery Area

UV light filters 2

UV light kills microorganisms