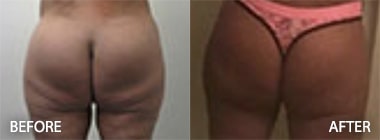
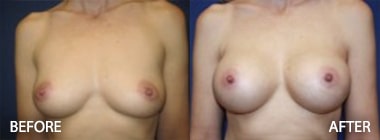
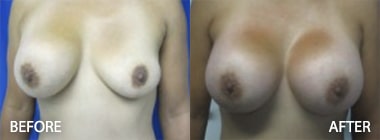
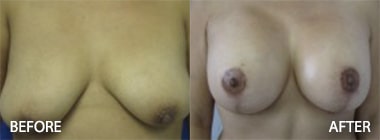
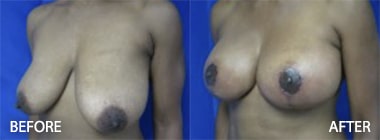
The Effect of Radiation on Complication, Reoperation and Capsular Contracture Rates in Implant-Based Breast Reconstruction Following the Introduction of Skin-Sparing Mastectomy (SSM) Techniques
Introduction
Mastectomies have implications for the psychosocial well being of the patient and every attempt should made to reconstruct the breast in suitable patients.(1) Skin-sparing mastectomy (SSM) is one of the techniques developed to improve the aesthetic result of breast reconstruction. The concept of pre-operative plastic surgery planning together with SSM was first brought to the forefront by Toth(2) et al. in 1991. It involves the preservation of a native skin envelope with the removal of the breast, nipple-aerolar complex, biopsy scars and skin overlying any superficial tumours. (2) The ideal SSM would have a skin flap devoid of all breast tissue but contained adequate blood supply to prevent flap necrosis and delayed wound healing. It is believed that the preservation of the skin architecture and intact infra-mammary fold allowed for immediate breast reconstruction thereby reducing the number of reoperations and improving the cosmetic appearance of the breast.
For many years, the expander/implant option was not available as a reconstructive option post mastectomy and autologous tissue was the mainstay of treatment. Various studies also suggested that tissue expansion were associated with a significantly higher complication rate.(3-5) In fact, one study by Kroll and Baldwin(4) reported in their 325 post-mastectomy reconstruction patients, that the failure rates for tissue expansion was as high as 21% whilst their TRAM flap suffered a mere 3% failure rate. Other studies have been more favourable of implants with one study by Rosen and colleagues(6) finding that the complication rates were similar between TRAM and tissue expander/implant reconstruction for breast reconstruction.
While there are studies which have demonstrated the efficacy of SSM and autologous reconstruction,(5) SSM with expander/implant reconstruction has been evaluated little in the literature. A PubMed search of “skin sparing mastectomy” AND “tissue expansion” OR “implant” revealed 30 original articles with the first articles of any relevance being published within the last 10 years.
This study explores the outcome of breast implants following conservative mastectomies and SSM. It also examines the complication and reoperation rates in patients who have undergone delayed versus immediate reconstruction as well as patients who have and have not undergone radiation therapy. The main hypothesis is that that there is no difference in outcome between patients undergoing SSM versus conventional mastectomy. The secondary hypotheses include that there is no difference in complication rate in patients undergoing delayed versus immediate reconstruction but an increased complication rate in patients who have had radiotherapy to the affected breast and axilla.
Methods
A retrospective chart review was performed on 132 patients undergoing 227 implant-based breast reconstructions over a 4 year period (2006-2009) at the University of Kansas Medical Centre. The senior author performed all of the reconstructions and follow-up which ranged from 12 to 36 months post-operation. All patients had reconstructions with either Mentor ( Irving, USA) or Inamed/Allergan ( Irvine, USA) expanders (subpectoral) together with either a skin-sparing mastectomy or conventional mastectomy. The creation of sling was performed with Alloderm (LifeCell, Branchburg, USA), FlexHD (Ethicon,??) , Neoform ( Mentor, Irving, USA), or Strattice (LifeCell, Branchburg, USA. No attempt was made to standardize initial fill volumes, time to full expansion, or final volumes achieved
Data collected included type of surgery (immediate versus delayed, skin-sparing versus conventional mastectomy), history of radiotherapy treatment and complications. Complications include re-operation, capsular contracture, infection, seroma formation, post-operative haematoma, implant exposure and delayed wound healing. The modified Baker classification of capsular contracture(7) was used. All personal identifiers were removed from the data as stipulated Human Subjects Review Committee. Results were recorded and tabulated using Microsoft Access. Chi-square tests were performed on the data, and p–values were used to evaluate the data for statistical significance.
Results
A total of 132 patients received 227 mastectomies, of which 64% (145 patients) had conventional mastectomy skin envelope excisions, 33% (75 patients) were SSMs and 3% (7 patients) were of Wise pattern excisions. The average age of patients was 52 years with the following ethnic breakdown: 84% White, 5% African-American, 5% Hispanic, 1% Asian and 5% other. 2% were current smokers, 18% had a history of smoking, and 80% were nonsmokers. 8% of the patients were diabetic. With regard to radiation exposure in this study, 12% had a remote history (>1 year removed from surgery), 9% had immediate preoperative radiation, and 15% had postoperative radiation.
The overall complication and re-operation rates were 15% and 10% respectively. (Figure 1 and 2) Of the patients who had infected implants, half were managed conservatively with antibiotics whilst the remaining half of the infections necessitated surgical removal of implants. 75% of implant exposures (6/8) were treated with removal of implant, whilst the remaining 25% received irrigation and closure. Finally, 2 of the 3 hematomas required surgical drainage.
Skin-sparing vs. Conventional Mastectomy
Overall the SSM group had a lower complication rate (12% vs 18%) but a greater re-operation and capsular contracture rate than the conventional mastectomy group (Figures 3 and Table 1). Of these, only the reoperation rate was statistically significant. (p<0.01)
Immediate vs Delayed
Delayed breast reconstructions were associated with a significantly greater number of reoperations (p< 0.0001) than immediate reconstructions, but the overall complication rates were similar (Figures 4 and Table 2). The immediate group showed a higher rate of capsular contracture (5% vs. 0%), although this difference was not statistically significant (p=0.21).
Influence of Radiation
The irradiated group had higher rates of complications and re-operations (Figure 5 and Table 3), but only the rate of reoperation between the two proved significant statistically (p=0.02). Capsular contraction was similar between the two groups.
Discussion
The field of implant-based reconstruction is constantly undergoing change. These include the advent of dual chambers, anatomic and cohesive variations, texture modifications, and ever evolving proprietary manipulation. As a result, implant-based reconstruction data will remain difficult to standardize over any prolonged periods of time. Similarly, size of implant, initial volumes, final volumes, and rapidity of expansion are tailored to meet patient goals and expectations and can never fully be standardized. The development of skin-sparing and, more recently, nipple-sparing techniques also adds a distinct element to the gamut of variability.
The overall complication rate of our implant-based reconstruction was 15% and a reoperation rate of 10%. This is fewer than that reported by Rosen et al in 1990 who had a complication rate of 23 their tissue expander and compared to and 24% for TRAM flap reconstructions.(6) It is also much lower than the rate reported by a large study of 165 immediate reconstructions in 1986 by Bailey et al. They had a 22% implant and 15% expander loss and an overall complication rate of 57%.(8) This may reflect not only the difference in the implants and expanders itself but also a learning curve where it is presumed that over the last 30 years, surgeons have improved technique with time.
Breast reconstruction may be performed immediately post-mastectomy or delayed for up to years following the initial mastectomy. Immediate breast reconstruction is often recommended for the psychosocial benefits,(1) but obviously, this needs to be weighed against the patient, the surgeon and oncological needs (including further operation and adjuvant radiotherapy). This study has demonstrated that not only are implant based reconstruction associated with a low complication rate, but immediate reconstructions are also associated with statistically significant lower reoperation rate.
There are two major concerns regarding implant reconstruction following SSM. The first concern is that most breast reconstruction occur in the anterior chest skin(1) and therefore SSMs may increase the risk of recurrence. The breast surgeon must balance between the risk of skin necrosis in the residual skin flap and the risk of recurrence if breast tissue is left behind in the SSM flap. A multitude of studies have demonstrated that there are no difference in local recurrence rate and overall survival between mastectomy and reconstructed groups.(1) Secondly, studies have shown that there is a severe complication rate approximately 20% in patients who undergoes immediate implants post SSM.(9-11) Other studies have suggested that carefully selected patients could result in a complication rate as low as 5%.(12) Our studies complication rate was at the lower end of that reported in the literature, again perhaps reflecting the learning curve in the skin-sparing paradigm.
Overgaard et al’s landmark trials in 1997(13) has resulted in radiation therapy becoming increasingly used as adjuvant therapy to reduce local recurrence rate, prolong disease free and increase overall survival rate.(1) One would expect post-irradiated breast to be associated with higher postoperative complication due to radiation associated damage to surrounding tissues.(1) Some researchers have classed patients who have had irradiation to be similar to heavy smokers and have recommended SSM to be avoided in such patients.(9) Other studies have been shown that radiation therapy is associated with unacceptably high rate of capsular contracture and rupture of the implant envelope or capsule.(1, 14, 15) This include one study by Spear in 2000 of 40 consecutive patients undergoing staged expander/implant placement and radiation during a 7 year period demonstrated that capsular contracture rate was 21% in the radiated vs. 0% in the control group. (16) However, our study has not shown this. One could argue that as capsular contracture develops over months to years, and this study does not have the long-term follow-up to evaluate the overall contracture rateSpear’s study also reported complications to be more common in the irradiated group (36%) than in the control (7%).(16) The infection rate was also higher at 4% in the irradiated group and 0% in the control group. (16) Finally, 32% of radiated breasts with implants ultimately needed the addition of a flap.(16) Our study has demonstrated somewhat different results, with irradiated breasts having a statistically higher re-operation rate, but similar rate of complication than non-irradiated breasts. . It could also be due to improvement in the targeting of irradiated beams to limit damage to surrounding tissue, improved surgical techniques or quality of implants.
A word of clarification should be entered on the nature of the capsular contracture. None of the patients were observed to have any greater than Baker Grade II capsular contracture, and the overwhelming majority could be classified as Grade I. An additional group of patients remain in relatively early follow-up period after implant placement (<6 months). (???? – this is from the original paper) As such, capsular contracture rates from this group were excluded from all calculations.
The study has a few limitations in addition to the nature of the topic, which has already been delineated. The most obvious limitation is its retrospective nature. Although ideally, patients would be prospectively randomised to the various subgroups, the study would not be an ethically sound. Secondly, follow-up was variable, with most patients being followed from 1 to 3 years. A follow-on study of patients 5-10 years post-operatively would be of value in identifying the long-term effects of the various subgroups. Thirdly, while the conventional mastectomy group could function as its own control from the SSM group due to temporal overlap, the two groups were not of equal size and no attempt was made to match them. However, again it would be difficult to design, even prospectively due to the patient’s individual requirements. Finally, though only one surgeon performed the reconstructions and the follow-up, two surgeons performed the mastectomies. This could potentially create discrepancies in flap thickness and viability and, ultimately, could have affected complication and reoperation rates.
Conclusion
While acknowledging this state of flux, the goal of this study was to determine complication, reoperation, and capsular contracture rates in implant-based reconstruction and the effect of radiation as a skin-sparing paradigm evolved at the University of Kansas Medical Center. While the study showed a trend toward SSM being associated with a lower complication rate compared to conventional mastectomies, the study did not show a positive effect on reoperation rate or rate of capsular contracture. Radiation exposure negatively impacted reoperation rates but oddly showed no increase in capsular contracture and overall complication rates. The complication, reoperation and capsular contracture rates are lower than what has been traditionally reported in the literature, and may reflect the increased surgical expertise, more targeted radiation therapy and improved implants being used in the patients. Immediate reconstruction with implants in patients who have undergone SSM, even in irradiated tissue, appears to be a viable option in breast reconstruction.
Article 1: The Role of Telemedicine in the Management of the Cosmetic Surgery Patient
Article 2: Breast Implant Reconstruction after Radiation
Article 3: Breast Reconstruction after Mastectomy
Article 4: Protocol for the Management of Keloid Scars
Article 5: Melanoma and the Role of Sentinel Lymph Node Biopsy
Article 6: Desmoid tumors of Bilateral Breasts
Article 7: The Role of the Paramedian Incision
Come to Hughes Plastic Surgery in Los Angeles and Beverly Hills. You will be glad that you did.