Jump To:
- DR. HUGHES BEST EYELID SURGERY DOCTOR IN BEVERLY HILLS
- PRINCIPLES OF YOUTHFUL RESTORATION IN UPPER AND LOWER EYELID SURGERY
- HISTORY AND EXAM IN UPPER AND LOWER EYELID SURGERY PATIENTS
- WHAT IS THE COST OF EYELID SURGERY
- TRADITIONAL UPPER AND LOWER EYELID SURGERY TECHNIQUES
- PRESERVING EYELID SHAPE AND TONE IN EYELID SURGERY
- THE TRANSCONJUNCTIVAL (SCARLESS) EYELID SURGERY
- COMPLICATIONS OF UPPER AND LOWER EYELID SURGERY
- EYELID PRE- AND POST-OP INSTRUCTIONS
Dr. Kenneth Hughes has a multitude of techniques to address your aging eyes with a variety of upper and lower eyelid surgeries in Los Angeles and Beverly Hills. Dr. Hughes has extensive facial cosmetic experience in eyelid surgery and blepharoplasty following his Harvard Medical School aesthetic fellowship.
Dr. Kenneth Hughes Has Performed Hundreds of Eyelid Surgeries in Los Angeles and Beverly Hills, CA
Upper and lower eyelid droopiness, fat bulging, and wrinkling are frequently the first signs of facial aging. Dr. Hughes can perform correction of the both eyelids (blepharoplasties) together or separately depending upon patient preference and needs. These are frequently performed in conjunction with face and neck lift and/or brow lift to improve the entire face. Upper and lower eyelids can be performed on an outpatient basis in less than one hour.
The upper and lower eyelid surgeries remove excess skin and fat that may have developed as a result of heredity or during the aging process. The scars are hidden in natural skin crease for the upper eyelid procedure. The scars are hidden in the shadow of the lash line for the lower eyelid procedure. Upon scar maturation, the scars are virtually undetectable.
Dr. Kenneth Hughes Voted Best Eyelid Surgery Doctor in Los Angeles and Beverly Hills, CA
Principles of Youthful Restoration in Upper and Lower Eyelid Surgery
The upper eyelids and the relative skin excess in this area must always be evaluated in relation to brow position. Brow position should be corrected first before upper eyelid skin removal is considered. In many patients, brow lift can eliminate the need for upper eyelid surgery. However, in the majority of patients with facial aging complaints, patients should receive both upper eyelid surgery and a brow lift.
Brow lift is not being performed as commonly as it was only a few years ago. Coronal, endoscopic, temporal, and direct brow lift may be good options in the appropriate patient. Dr. Hughes will help you sort these issues out during the consultation.
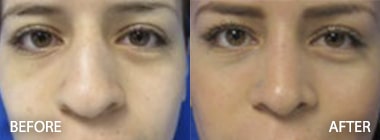
In the upper lid, there should be a well-defined lid crease. Surgery helps to restore this crisp fold. In addition, hooding at the lateral aspect of the upper eyelid can be corrected as well. Those patients with fullness medially in the upper eyelids can have some of the fat pads removed.
In the lower eyelid, removal of the some of the fat often makes a reduction in the appearance of bags or fullness in the lower eyelids. In addition, skin wrinkles can be improved by removing some of the skin of the lower eyelids. Finally, it may be necessary to restore the tone of the lower eyelids. If this is not done, the patient may have a sad appearance or look older. In addition, the patient may be at risk for lid malposition. Dr. Hughes will discuss with you during your consultation if your tone needs to be improved with a technique called lateral canthopexy or lateral canthoplasty.
History and Exam in Upper and Lower Eyelid Surgery Patients
History for Upper and Lower Eyelid Surgery
Patients should not be taking medications that are anticoagulants such as anti-inflammatory and cardiovascular drugs and vitamins (especially vitamin E ). Herbal supplement use should be discontinued. Hernal preparations can present risks to anesthesia and surgery, particularly those affecting blood pressure, blood coagulation, the cardiovascular system, and healing.
Dr. Hughes will ask you specific questions about your medical history, especially hypertension, diabetes, cardiovascular and cerebrovascular disease. He will ask about problems with bleeding or clotting.
Patients should stop smoking one month prior to surgery.
Contact lens wearers should discontinue contact lens wear before surgery if there is any question and leave the lenses out for at least 2 weeks after surgery to allow healing without the need to manipulate the eyelids.
Patients who have LASIK or similar procedures are at greater risk for dry eyes.
Preoperative Exam for Blepharoplasty (upper and lower eyelid surgery)
Dr. Hughes will assess the shape of the eyes. He will point out prominence or asymmetry of the globes. He will examine for evidence of exposure, dryness, or “injection” of vessels. He will check to make sure that you can completely close your eyes.
He will check the tone of the lower lids by pulling the lid away from the globe and releasing them. He will also test how quickly the lower lid returns to position after depressing. In addition, Dr. Hughes will evaluate for presence of herniating fat.
What is the Cost of Eyelid Surgery in Los Angeles?
- Eyelid, Lower (Blepharoplasty) – $6500
- Eyelid, Upper (Blepharoplasty) – $4000
Please note that pricing for Eyelid Surgery may vary based on the individual needs of the patient.
Traditional Upper and Lower Eyelid Surgery Techniques
The traditional upper blepharoplasty commonly must be combined with a brow elevation operation to balance the brow drop that often results from upper eyelid skin removal. The upper eyelid or blepharoplasty incision is marked according to how much tissue will be retained after excision between the upper incision and the eyebrow and the lower incision and the lid margin. The remaining tissue between these designated areas is the amount that can be removed safely and keep the eyelid crease in the proper line. After excision of the excess skin and muscle as a single unit, the orbital septum is opened, and the fat from the medial and middle compartments is teased out. All of the redundant fat freely protruding beyond the orbital septum is removed by electrocautery of the base. At that point, the closure is performed with a skin stitches. The incision and subsequent scar is hidden in the upper eyelid crease.
The lower eyelid surgery or lower blepharoplasty frequently involves removing skin, muscle, along with subtotal resection of the three lower eyelid fat pads. The fat can be transposed into the tear trough to ameliorate that area. The incision and subsequent scar is hidden under the eyelashes.
Preserving Eyelid Shape and Tone in Eyelid Surgery
If lower eyelid tone is poor, Dr. Hughes may advise the patient to have a lateral canthopexy or canthoplasty. This procedure involves placing a stitch in the lateral canthal tendon and repositioning it higher and farther back . A lateral canthopexy not only will help to prevent the complications of retraction of the lower eyelid after blepharoplasty but also establishes an aesthetically and functionally youthful eyelid. A properly executed canthopexy restores the tone, posture, and tilt to the lower eyelid. With restoration of the normal intercanthal axis tilt, lid tone, and septal integrity, the appearance of excess skin and herniated fat can be improved.
In the appropriate patient, lateral canthopexy or canthoplasty will preserve the long-term benefits of blepharoplasty, prevent complications, and restore youthful aesthetics.
The Transconjunctival (Scarless) Eyelid Surgery
Transconjunctival blepharoplasty involved making an incision inside the lower eyelid by everting the lower eyelid. This lower eyelid surgery approach allows for the creating of an essentially scarless approach. This lower eyelid surgery approach is the preferred procedure for fat reduction in patients without excess skin and with good canthal position.
This approach minimizes but does not eliminate postoperative lower lid retraction and malposition. Occasionally, a lateral canthopexy or lateral canthoplasty stitch can be placed if necessary.
Complications of Upper and Lower Eyelid Surgery
Patients generally look presentable approximately 2 weeks after surgery. On occasion, prolonged edema or bruising can be an issue. Generally, these items are managed conservatively. Occasionally, Dr. Hughes may place a tarsorrhaphy stitch or Frost stitch to support the eyelid during healing.
Postoperative infections are uncommon.
The most feared complication is the retrobulbar hemorrhage. Any complaint of severe orbital pain needs to be examined immediately, especially that of sudden onset. Any significant decrease in vision with progressive proptosis is of significant worry. The treatment of this problem involves release of sutures and release of the lateral canthus to relieve pressure. The eye should be explored in the operating room to determine if any vessels continue to bleed.
Lid malposition or ectropion (retraction with eversion of eyelid) can occur following lower eyelid surgery due to a variety of issues, both technical and healing dependent. Conservative treatment and eye lubrication are utilized first.
Dry eyes can be a problem after upper and lower eyelid surgery, but the vast majority resolve without intervention. Artificial tears can be used as a temporizing measure.
Recovery From Eyelid Surgery
The recovery process is short for the eyelid procedures (blepharoplasties), including a few days of minor bruising and swelling with return to work shortly therafter. The results of eyelid surgery frequently last for a decade or more.
Frequently, the eyelid surgeries produce nice, age defying results without any complications. Those with poor eyelid tone may need additional suture techniques called canthoplasties or canthopexies to tighten the lower eyelid. These people are also at greater risk for lid malposition, ectropion (or lid eversion), and dry eye symptoms. Dr. Hughes will discuss with you the risk category into which you fall.
Eyelid Surgery Photo Galleries of Dr. Hughes

Eyelid Surgery
BEFORE & AFTER GALLERY
Dr. Kenneth Hughes, MD has a multitude of techniques to address your aging eyes with a variety of upper and lower blepharoplasties (eyelid surgeries).
View Articles from Upper and Lower Eyelid Surgery Article Library Below:
Article 1: Principles of Youthful Restoration in Upper and Lower Eyelid Surgery
Article 2: History and Exam in Upper and Lower Eyelid Surgery Patients
Article 3: Traditional Upper and Lower Eyelid Surgery Techniques
Article 4: Preserving Eyelid Shape and Tone in Eyelid Surgery
Article 5: The Transconjunctival (Scarless) Eyelid Surgery
Article 6 : Complications of Upper and Lower Eyelid Surgery
Eyelid Pre- and Post-Op Instructions