Jump To:
- WHAT ARE JOWLS AND HOW CAN THEY BE REMEDIED?
- ADDRESSING A LOOSE OR SAGGY NECK
- WHAT IS THE COST OF LOWER FACE/NECK LIFT
- WHAT ARE MARIONETTE LINES AND HOW ARE THEY TREATED?
- THE TREATMENT OF THE NASOLABIAL FOLDS
- SKIN-ONLY FACELIFTS
- DEEP-PLANE FACELIFT
- SMAS-PLATYSMA FLAP
- EXTENDED SMAS-PLATYSMA TECHNIQUE
- SMASECTOMY
- SMAS IMBRICATION
- MACS LIFT
- FACELIFT COMPLICATIONS
- OPTIMAL SCAR PLACEMENT
- FOLLOW-UP AND RECOVERY
- FACELIFT REVISIONS
- LIP REJUVENATION
- LASER RESURFACING FOR STATIC WRINKLES
- COMPLICATIONS OF RESURFACING
- ADDITIONAL READING
- PRE-OP INSTRUCTIONS
- POST-OP INSTRUCTIONS
- ARRANGING A CONSULTATION
Dr. Kenneth Hughes has performed short scar facelifts for patients in Los Angeles and Beverly Hills for over a decade. The results can be dramatic or subtle. Dr. Hughes possesses a very rare talent for facelifts following his aesthetic fellowship at Harvard Medical School.
For facelifts, Dr. Hughes typically makes only an incision hidden around the ear (periauricular incision). The incision does NOT extend into the forehead or into the hairline.
The hairlines are not shifted as you may see in other facelift procedures. Dr. Kenneth Hughes is able to get natural results without giving away that something has been done. Many famous models, actors and personalities have had facelifts — some are easy to identify, some are not.
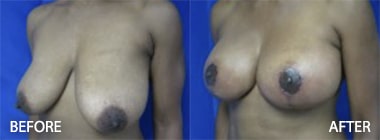
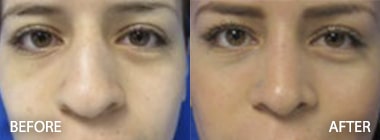
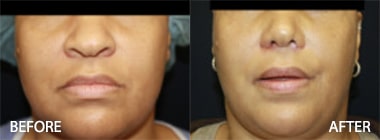
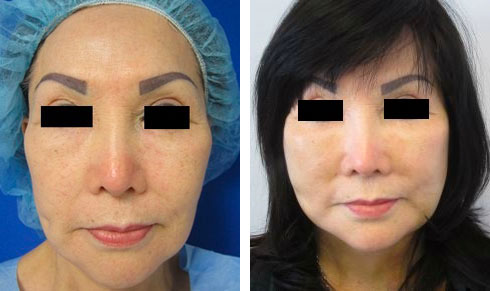
Look at the before and after photos under the facelift gallery. The cheeks are natural as are the necks and jowls. The scars are imperceptible. The ears appear unaltered. There is no wind-blown look, and Dr. Kenneth Hughes’s patients do not appear pulled or frozen.
Typical recovery is about 1 week of bruising and swelling, which varies from person to person. There is very little pain associated with the procedure.
Why Have a Facelift?
The facelift is a very common procedure to remedy signs of facial aging. Patients may complain of loose skin on the neck, hanging necks, or turkey necks. Patients may complain of saddened faces, jowls, falling jawlines, and falling or deflated cheeks. Frequently, people with signs of facial aging want to address their wrinkles or folds, particularly the nasolabial folds and marionette lines. Dr. Kenneth Hughes also utilizes facial fat grafting with his facelifts in Los Angeles.
In addition to a facelift, Dr. Kenneth Hughes may recommend upper and lower eyelid surgery (upper and lower blepharoplasty) or a brow lift to complete your transformation.
WHAT ARE JOWLS AND HOW CAN THEY BE REMEDIED?
Jowls are descending, fibro-fatty deposits that accumulate along the inferior border of the mid-mandible. The jowl formation is the result of masseteric cutaneous ligament laxity, which develops in the cleavage plane between the superficial and deep fascia of the face. These jowls are best addressed with a facelift.
Direct excision of jowl fat can be performed. If a facelift is not planned, suction-assisted lipectomy with a small blunt cannula can be performed.
There are many facelift techniques that can address sagging jowls, but all successful techniques have in common ligamentous release and resuspension or fixation. This release can be sub-SMAS or supra-SMAS, but in both, the masseteric cutaneous ligaments are released in one plane. SMAS elevation with concomitant delivery of jowl fat into the face.
Another option for correcting the appearance of jowls is a mini facelift.
[…] I had a full facelift done just three short years ago here in Austin, Texas. The last year my lower face has literally fallen as if nothing had ever been done. […] I came to LA from Austin, TX, to meet with him and get his opinion about how to improve the lower face and neck. […] He is truly talented, and I could not be happier at my new fresh face in which people have a hard time believing I am 52! Look no further if you want the best!
Addressing a Loose or Saggy Neck
Mild to moderate skin laxity can be treated with minimal or no skin excision, whereas significant laxity requires skin excision. The amount of subcutaneous tissue and its location in the submental or subplatysmal space are determined.
Laxity and banding of the platysma muscle and prominence or thickening of the digastric muscle as well as ptosis of the submandibular gland should be noted. Vertical and sagittal microgenia must also be recognized – both hasten facial aging, and their correction may dramatically improve the surgical result.
For patients interested in rejuvenation of the neck only, one should generally adhere to the following treatment strategies: in the young patient (40 years or younger), liposuction alone will yield the best results most of the time.
In the middle-aged patient (40 to 55 years), submental lipectomy combined with anterior platysmaplasty (tightening of the muscles in the neck) can be performed.
In the elderly patient or patients with significant skin excess and laxity, submental lipectomy and direct excision of anterior neck skin can be performed.
What is the Cost of A Lower Facelift in Beverly Hills and Los Angeles?
- $20,000 to $35,000 or more depending upon the need for neck dissection, platysmal plication, and the overall skin laxity
Please note that pricing for Lower Face Lift (local or general) may vary based on the individual needs of the patient.
What Are Marionette Lines and How Are They Treated?
These lines extend from the oral commissures vertically down toward the chin. These consist of a complex combination of overlapping muscle structures, including the orbicularis oris, the depressor anguli oris, and the depressor labii muscles, in association with a vertically oriented series of fibrous bands (marionette cutaneous ligaments) attaching the lateral aspect of the muscle to the skin. This area is difficult to fully correct with any single technique and often requires a combination of approaches.
A facelift approach with undermining of the skin and release of the marionette cutaneous ligaments will improve this area, but the distance from the point of maximum pull to the affected area or marionette line often precludes full correction or can result in early recurrence.
Soft tissue augmentation with fillers, laser resurfacing, dermabrasion, and deep chemical peels work better on static rather than on dynamic lines. In rare instances, direct excision of lines can be performed.
The Treatment of the Nasolabial Folds
Deep nasolabial folds are especially troublesome after massive weight loss and in those patients with significant maxillary retrusion. Fibrous bands can be found attached to the underlying muscles, including the levator labii superioris, zygomaticus major and minor, labii superioris alaeque nasi, and risorius muscle.
The accumulation of fat lateral to the fold combined with the check-ligament effect of the fibrous bands leads to accentuation of the nasolabial fold. Augmentation of the area under the fold can be performed with an injectable filler such as Juvederm or Radiesse, which are temporary, or more permanently with facial fat grafting procedures.
If facelift surgery is in the rejuvenation plan of the patient, undermining of the fibrous attachments deep to the fold will provide some correction. When the fold is undermined, it is most effective to lay autogenous tissue, such as fat or de-epithelialized dermis, under the fold to prevent reattachment to the underlying musculature.
In older patients, especially men with deep nasolabial folds, direct elliptical excision can be performed. With this technique, the fold itself will not entirely disappear because it is a well-defined anatomic area. However, its depth will be less pronounced.
Skin-Only Facelift
The skin-only facelift can be initiated within the temple hair above the insertion of the helix or, alternatively, begins along the anterior temple hairline and encircles the sideburn to reach the helical insertion.
The incision continues in a gently undulating fashion, hugging the preauricular helical root, tragus, and around the lobe to continue on the postauricular skin. At that point, it may descend posteriorly along the hairline or may extend to within the hairline, depending on the degree of neck laxity and anticipated skin resection.
Although Dr. Hughes performs SMAS plication with skin resection for longer lasting results than skin-only facelifts, he performs shorter scar facelifts, which do not extend into the temple or the hairline.
Whereas the skin facelift exerts tension on the paralabial cheek and the lower anterior neck, only minimal tightening is transmitted to the submental region, and correction of the anterior jaw and submental areas is often suboptimal. Consequently, some method of direct approach to the submental area with medial platysma plication is added.
A submental incision is used for direct fat removal and tensioning of the platysma with midline plication sutures. The medial plication of the submental platysma tends to draw the laterally attached skin along the inferior mandibular border medially.
Most commonly, the vector line is approximately parallel to the inferior border of the mandible. Too much upward vector of lift on the cheek skin flap separates the skin edges of the superior part of the incision, making closure difficult.
An additional problem is excessive elevation of the temporal hair pattern. Too much lateral rotation of the postauricular skin flap causes problems of closure of the incision at the postauricular sulcus, which can cause excessive tension on the thin skin flap with poor healing.
Deep-Plane Facelift
“Deep plane” is a term applied by Hamra, who described dissection in the midface superficial to the zygomatic muscle beneath the mass of the cheek fat. The blunt finger dissection between the midface SMAS and the cheek fat liberated the descended malar fat pad, which was advanced laterally under “great tension” on the cheek skin flap.
The composite technique added a vertical vector of lift on the orbicularis oculi muscle through the lower blepharoplasty incision for enhanced improvement of the eyelid-midface complex.
The risk for facial nerve injury is much higher in this procedure than with other more conventional facelift techniques. This procedure has faded in popularity in recent years.
SMAS-platysma flap
Owsley developed the SMAS-platysma rotation flap technique, reasoning that laxity in the lower face and submental area was primarily due to loss of support from the SMAS and masseteric ligaments as well as loss of elasticity in the overlying skin.
Experience has shown that wide undermining and repositioning of the platysma-SMAS layer is the key to long-term repositioning of the anatomic features of the lower face and neck.
The principal advantage of the SMAS-platysma technique is the multiple vectors of lift that can be placed on the mobilized SMAS-platysma flap after complete undermining to the midline of the neck and beyond the masseteric ligaments in the cheek.
The vertical vector of tensioning applied along the SMAS incision at the zygomatic arch directly lifts the midmandibular jowl area and effects a snug tensioning of the submental region.
Extended SMAS-Platysma Technique
SMAS incision is begun in the preauricular region about 1 cm anterior to the skin incision and extends inferiorly from the superior tragal notch, which corresponds to the inferior border of the zygomatic arch, down to the level of the attachment of the earlobe.
The branches of the facial nerve are well protected beneath the substance of the parotid gland. An entirely safe dissection can be performed over the parotid with sharp scissors directed upward. A small cuff of SMAS tissue is left attached along the zygomatic arch to facilitate suture fixation.
The mobilized SMAS flap is then rotated upward with some posterior traction to accomplish the desired vector of lift of the lower face, jaw line, and neck based on the surgeon’s judgment.
SMASectomy
SMASectomy involves removing a portion of SMAS. The mobilized SMAS flap is then rotated upward with some posterior traction to accomplish the desired vector of lift of the lower face, jaw line, and neck based on the surgeon’s judgment.
The primary vector is upward, but a lateral component of tension is added to apply lifting of the labiomandibular fold. Sufficient SMAS tissue is excised to ensure a snug closure forward along the zygomatic arch, which will directly transmit a vertical lift to the platysma along the mid and anterior body of the mandible.
SMAS Imbrication
In 1997, Stuzin described SMAS imbrication. He also described periosteal fixation to arch with a strip of SMAS. The platysma is secured to mastoid fascia to pull neck tissues.
MACS Facelift
Tonnard developed the MACS (Minimal Access Cranial Suspension) lift with simple and extended versions. Simple MACS consists of limited skin undermining with 2 purse-string SMAS sutures of 2-0 permanent suture (Prolene) to the deep temporal fascia.
The extended MACS includes an incision that extends along the temporal hairline. The pull of the malar tissues is performed with a 3rd purse string suture secured to the deep temporal fascia.
Dr. Kenneth Hughes can and has performed all variants of facelift approaches described.
Facelift Complications
Hematoma is the most common facelift complication. Its incidence has been recorded in various series as ranging from 1% to 8%, with an average of about 4%. Discontinuation of medications such as aspirin and other non-steroidal anti-inflammatory drugs is paramount.
If the patient has high blood pressure, the blood pressure must be well controlled prior to the facelift surgery. The patient’s intraoperative and postoperative elevations in blood pressure and the occurrence of nausea and vomiting will be prevented to the extent possible.
Hematoma occurs in a disproportionately higher percentage of male facelift patients. In addition to the usual measures of hemostasis, blood pressure and pain control, careful observation must be intensified with the male facelift patient.
Early Hematomas
Acute expanding hematomas usually occur in the first 6 hours of the postoperative period. When the patient complains of pain and develops sudden increasing swelling often accompanied by increasing ecchymosis in the periorbital area, a hematoma is almost always present, and the dressings should be removed for better inspection.
If, as is common, the hematoma is localized in the postauricular and lateral neck area, an initial attempt should be made immediately in the recovery room to evacuate the hematoma with suction and to control the bleeding by applying local firm pressure for a time.
A long 3- to 4-mm-diameter liposuction cannula accomplishes the evacuation well when it is passed down between the postauricular sutures. The suction effectively removes the collected blood, and the pressure applied to the wound area combined with control of blood pressure elevation solves the problem most of the time.
Late Hematomas
Late hematomas typically occur between days 7 and 10 after a facelift. The bleeding is almost always arterial from an injured branch of the superficial temporal artery that reopens because of an abrupt elevation in blood pressure that dislodges a clot off the area of injury.
Patients must be cautioned about their activity for a full 2 weeks; they are required to abstain from any exertional activity that would elevate blood pressure, including sex. Surgical exploration of a late hematoma is almost always mandatory to locate and to ligate the bleeding arterial branch.
Infection
Infection in plastic surgery of the face is uncommon due to the generous blood supply of the head and neck tissues. The rare infection almost always follows the bacterial colonization of a small unsuspected hematoma. If an infected hematoma does occur, adequate drainage is mandatory along with cultures and aggressive antibiotic therapy.
Skin Slough or Skin Loss
Skin slough results from diminished circulation of the undermined skin flaps and usually occurs adjacent to the periauricular incision line. The primary cause of diminished circulation is excessive tension on the flap, which has to be judged at the time of closure by the surgeon.
Hematoma is certainly a factor in increasing the skin tension, and the presence of a systemic autoimmune disease or the chronic use of steroid medication can predispose to the occurrence of skin slough. Skin slough is 10 times greater in patients who smoke.
Closure of the skin flap is without any tension at all, but merely a redraping type of approach with appropriate trimming. After secondary wound healing, a subsequent scar revision can be done electively.
Nerve Injury
Undermining the facelift skin flaps interrupts the superficial sensory nerve endings, resulting in localized loss of sensation. Nerves take between 6 and 18 months before sensation is regarded as back to normal. This lack of sensation typically concerns patients quite a bit for the first 6 or 8 weeks and then seems to be less bothersome thereafter.
In a subcutaneous facelift, the branches of the facial nerve injured most commonly appear to be the frontal and the marginal mandibular. In the course of sub-SMAS-platysma dissection, the cervical branch has been the most frequently injured, followed by the marginal mandibular.
The frontal branch lies deep in the substance of the parotid gland until it reaches the caudal margin of the zygomatic arch. It is only after passing the cephalic margin of the zygomatic arch that the frontal branches penetrate the deep fascia and continue on the undersurface of the superficial temporalis fascia accompanied by branches of the superficial temporal artery.
Dissection at the plane between the temporalis fascia and the deep temporal fascia, which should be performed bluntly in the region 1 to 2 cm above the zygomatic arch.
Optimal Scar Placement in Facelift Surgery
The scar around the earlobe is perhaps the most important. The scar should not lie directly in the lobular-facial crease because the crease itself constitutes a delicate anatomic subunit that should not be disrupted.
A superior result will be obtained if the scar is situated a few millimeters inferior to this junction and an attempt is not made to join thin, soft earlobe directly with thick cheek skin. Also, it is imperative that not too much tension is placed to pull the earlobe inferiorly.
Dr. Hughes performs short scar facelifts and does not make incisions into the temporal hairline or the occipital hairline. Incisions within occipital scalp may result in an unnatural and intolerable absence of occipital hair and notching of the occipital hairline.
Also, the temporal incision will either leave a visible scar or shift the hairline unnaturally.
Dr. Hughes will explain to you if you will need a submental incision hidden in the chin crease to perform surgery on the front of your neck. You may only need liposuction, which will not require the incision.
Facelift Follow-up and Recovery
Dr. Hughes will see you the day following your surgery. He does not place drains so there is no need to be apprehensive. Your dressings will be removed and the result inspected. Your stitches will be removed in about one week. Bruising will be gone in about one week.
Facelift Revisions
Secondary facelifts are those facelifts in patients who have had plastic surgery performed before. These are usually more difficult and should be done by plastic surgeons who have done more facelifts in the past. Dr. Hughes has performed hundreds of facelifts, and he has the experience and technical know-how to help in these more complicated cases.
Dr. Hughes performs a lot of secondary and tertiary facelifts for patients who may have not been happy by a previous surgery or in patients who want a little better result as the face continues to age. No facelift is forever, and revisions after 5 to 7 years are the norm.
In the secondary facelifts, Dr. Hughes addresses the same issues as primary facelift such as nasolabial folds, labiomental folds, cheek ptosis, infraorbital hollowing, malar flattening, jowl laxity, subplatysmal fat accumulation, submandibular gland hypertrophy, and cervical band formation.
In addition, if the first facelift was limited and consisted of skin excision and skin tightening only, Dr. Hughes performs a deeper, longer-lasting facelift. Dr. Hughes can also address scar and hair malposition issues. Windblown looks can be addressed as well. Pixy ears, where the ear lobes are pulled too far inferiorly, can be remedied as well.
Lip Rejuvenation or Lip Lift
The central lip lift procedure lifts the lip through incisions underneath the nose. Dr. Kenneth Hughes typically hides the incision within the nose and may not even make a central cut if unnecessary.
Some plastic surgeons perform these lifts with incisions that can be noticeable, and this procedure decreases the distance between the nose and lip. The central lip lift is only indicated in those patients with a vertically long lip.
One can also perform vermilion border excisions and corner of the lip lifts, all of which leave visible scars. Fillers such as Juvederm are used more commonly today as well as CO2 laser resurfacing and dermabrasion for perioral wrinkles.
Laser Resurfacing for Static Wrinkles
Laser resurfacing with the CO2 laser can be used to treat static wrinkles. First, prolonged recovery and erythema can be problems, especially in Fitzpatrick I and II skin types. Hypopigmentation is a function of the depth of injury rather than of the modality of treatment.
Complications of Laser Resurfacing
Scarring, hypopigmentation, hyperpigmentation, infection, reactivation of latent herpes virus infection, skin thickening or color changes can all occur after laser resurfacing.
All patients undergoing resurfacing in the perioral region should receive prophylactic antivirals, regardless of their past history of herpes infections. lncreased depth of injury will increase not only the elimination of deep rhytids but also the complication rate.
It is better to retreat an area 6 to 12 months after an initial resurfacing procedure than to manage complications.
Click on the Additional Face and Neck Lift Article Links Below to Learn More about Facelifts:
Article 1: Lip and Marionette Line Improvement in Facelifts
Article 2: Laser Resurfacing and Treatment of Nasolabial Folds in Facelifts
Article 3: Jowl and Neck improvement in Facelifts
Article 4: Skin Only Facelifts
Article 5: Deep Plane Facelifts and Extended SMAS Flap Facelifts
Article 6: SMASectomy, SMAS imbrication, and MACS Facelifts
Article 7: Complications of Facelifts: Hematomas
Article 8: Complications of Facelifts: Infection, Skin Loss, and Nerve Injury
Article 9: Optimal Scar Placement in Facelifts
Article 10: Secondary Facelifts
View Dr. Hughes’s Textbook Chapters Relevant to Facelifts
Chapter 3: Facelift
Chapter 2: Photography in Plastic Surgery
Chapter 1: Preoperative Workup in the Plastic Surgery Patient
Face Lift Pre- and Post-Op Instructions
Scheduling Your Facelift Procedure
Want to learn more about what a facelift can do for you? If so, contact our office and arrange a consultation with Dr. Hughes.